[ad_1]
This spring, at the height of the coronavirus pandemic, occupational therapist Rachel Wallbank was juggling three different roles.
In addition to being posted to work in the Covid-19 Patient Field Hospital at Principality Stadium in Cardiff and an acute care ward in support of those who had just been discharged from ICU, Wallbank was also trying to keep up with his aspects work as a clinical specialist in multiple sclerosis.
“[Covid] patients have had a significant infection, often with life-changing problems, “he says.” Probably the fantastic doctors and nurses saved their lives, but we care about the quality of that life they saved; it must be more than saving a life, [but building] one that has meaning for that individual. “
Wallbank is one of 41,000 occupational therapists (OTs) in the UK working in the fields of health, social care, housing and education, helping people with physical or mental illness, injury or disability to experience their life as completely as possible.
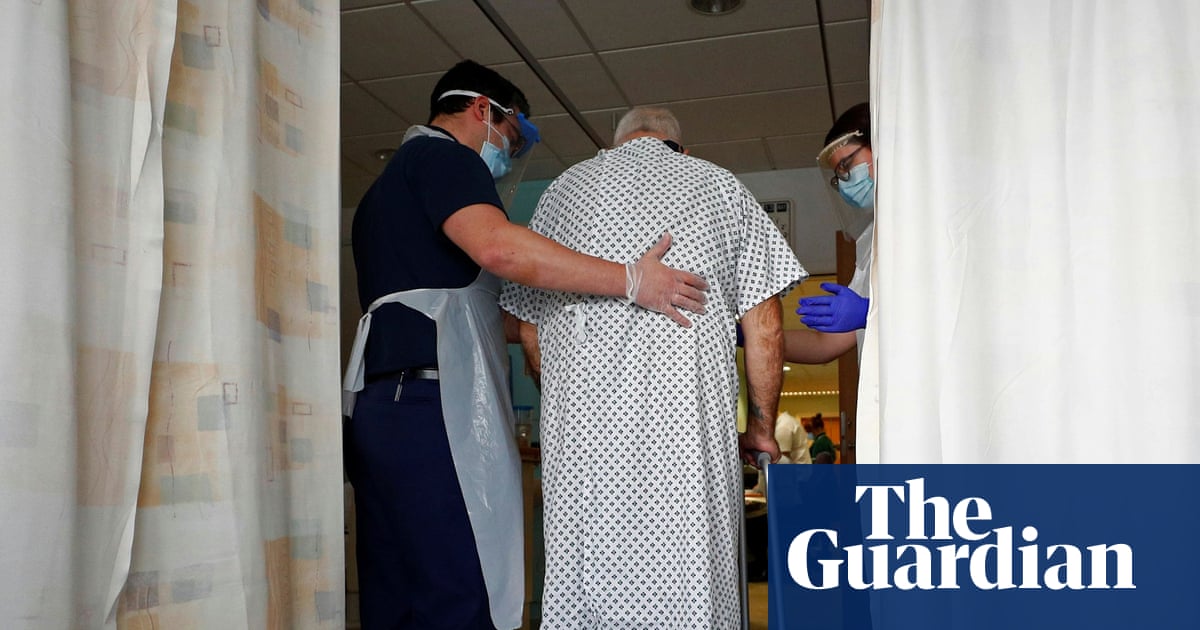
In the Welsh Field Hospital, Wallbank’s role was to support patients with washing, dressing, eating and moving around and helping them prepare for transfers. In the hospital ward, meanwhile, he was also helping his patients manage the fatigue and concentration problems brought on by Covid.
Lauren Walker, a professional advisor to the Royal College of Occupational Therapists, says OTs, like other frontline professionals, have been hugely affected by the pandemic.
A college survey of 1,500 professionals and students across the UK found that 98% of respondents said their work was affected in some way. A third was redeployed to other teams, and 60% were providing services differently due to Covid, such as switching to work online instead of seeing patients face to face.
Half of the respondents also said their work-life balance was affected and 46% said their health and well-being were adversely affected by the pandemic.
Catherine Murchan is one of four OTs working on the Acute Home Care team in the Southern Health and Social Fund in Northern Ireland. The team’s goal is to keep patients, mostly elderly, at home when they fall ill.
During the first wave of the pandemic, he says, the team felt fear and anxiety about their work, including concerns about the availability and effectiveness of personal protective equipment. He found a physically and emotionally strenuous job.
At first, they tried online and telephone assessments. “But we quickly realized that because our patients were seriously ill, they might get worse, be unable to get out of bed, be unable to climb stairs, and caregivers may have difficulty.”
Murchan’s team realized face-to-face input was essential and adapted working practices to keep professionals and patients safe.
Referrals to his team during the first wave increased by around 80%. Between March and the end of May, they saw around 350 people – a fifth of them Covid positive – in their homes and nursing homes. “Many patients wanted to avoid hospitalization,” he says. “They wanted to stay at home and their families would have preferred them to stay in their family environment.”
He says he has demonstrated his team’s resilience this year. “The staff generally felt very well supported and they felt that at that time we were all really united, we supported each other,” he says. “The fact is, in the second [wave] will everyone have the energy to carry on? “
As the country prepares for a second spike in cases, Murchan and his team are bracing by doing research on Covid treatment and rehabilitation. They are also concerned about what she calls a “deconditioning pandemic” among non-Covid patients who missed appointments during the first block, or didn’t exercise as much because they were protecting or chose to spend more time indoors.
Wallbank says OTs will also be at the forefront of Covid treatment for a long time and thinks a real picture of the virus’ consequences may not be clear for years. “I expect there will be a flood of individuals who have things like myalgic encephalomyelitis, post-viral syndrome and fatigue,” he says.
OT Chris Wood, based in Leeds, worked in a mental health ward during the lockdown and has now started a new job supporting the homeless. One of the biggest challenges for him during the second wave will be trying to keep the sleepers of the city safe.
“They don’t have access to the things we take for granted, like masks and hand sanitizers,” he says, “They don’t have access to news updates to get information and directions on what to do, and of course they don’t have a safe space to protect themselves. or self-isolate. “
Despite the challenges facing OTs and their clients, Walker thinks the profession has proven its worth during the pandemic and believes its profile has been improved.
Wood hopes it is. “Given how interesting, broad and innovative OT is, it’s surprising that people aren’t aware of it,” he says. “We sit in the background. We are a humble profession. Everyone knows what a nurse is and they probably know what a paramedic is. And then there are all these other professions like OT that offer so much. “
Source link